Polysomnography is a sleep study that helps doctors find sleep problems. You can do it at a sleep center or home.
In this article, we’ll talk about why someone might need this test and what happens during it.
Table of Contents
- What is Polysomnography?
- How common are sleep studies?
- When is a sleep study necessary?
- How do I prepare for a polysomnography?
- What happens during a polysomnography?
- What happens after a polysomnography?
- What are the risks associated with Polysomnography?
- How much does Polysomnography cost?
- Who does a sleep study?
- At-home sleep apnea testing vs Sleep Study
- What do the sleep study results mean?
- FAQs
What is Polysomnography?
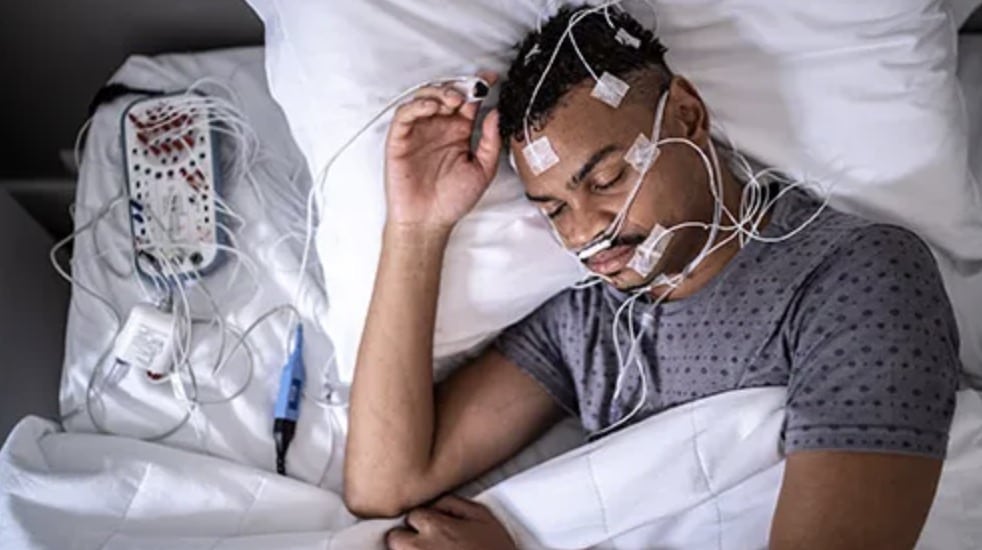
Polysomnography (PSG) is a test where you sleep while doctors watch and record data about your sleep patterns. They measure things like brain waves, muscle activity, oxygen levels, heart rate, breathing, and eye movement. This helps them see how you move between different sleep stages, like REM (when you dream) and non-REM (light and deep sleep).
By tracking these cycles and how your body reacts, doctors can spot any sleep problems you might have.
How common are sleep studies?
Sleep studies are done a lot. In 2014, over 800,000 were done for people on Medicare alone. And that’s not even counting those not on Medicare.
When is a sleep study necessary?
A sleep study helps doctors figure out what’s going on when you’re having trouble sleeping. They suggest it when you show signs of conditions that mess with your sleep. It helps them decide on the best way to treat these issues or to check if the treatments they’ve tried are working. These conditions mess with your brain, nerves, breathing, and heart. Some things a sleep study can find include:
- Sleep apnea (when you stop breathing during sleep)
- Narcolepsy (sudden, uncontrollable sleepiness)
- Restless legs syndrome (feeling the urge to move your legs at night)
- Insomnia (trouble falling or staying asleep)
- Certain types of seizures and epilepsy
- Night terrors (frightening dreams or screaming during sleep)
- Nocturnal panic attacks (sudden fear attacks at night)
- Sleepwalking or other weird sleep behaviors
- Sleep paralysis (can’t move when you’re waking up or falling asleep)
- Other types of sleep problems that mess with your sleep pattern
How do I prepare for a polysomnography?
To get ready for a polysomnography (PSG) test:
- Avoid alcohol and caffeine in the afternoon and evening before the test. These can mess up your sleep and affect the results.
- Don’t take any sedatives.
- Talk to your doctor about any medications you’re on. They might ask you to stop taking them before the test.
What happens during a polysomnography?
Here’s what happens during a polysomnography, which is a test done to check your sleep:
-
Setting: You go to a sleep center or a big hospital in the evening, a couple of hours before your usual bedtime.
-
Sleeping Over: You spend the night at the sleep center in a private room. You can bring your own stuff for bedtime, like pajamas.
-
Monitoring: A technician watches over you while you sleep. They can see and hear you through cameras and microphones in your room. You can also talk to them if needed.
-
Measurements: The technician keeps track of several things:
- Your brain waves
- Eye movements
- Muscle activity
- Heart rate and rhythm
- Blood pressure
- Blood oxygen level
- Breathing patterns, including any pauses
- Body position
- Limb movements
- Snoring and other noises
-
Sensors: They stick small sensors, called electrodes, on your scalp, temples, chest, and legs. These sensors are attached with sticky patches and are connected to wires.
-
Belts and Clips: Elastic belts around your chest and stomach monitor your breathing and chest movements. A clip on your finger measures your blood oxygen level.
-
Data Collection: All the data from the sensors goes to a computer through thin wires. Some centers also record a video to see how your body moves during the night.
-
Sleep Comfort: You might not sleep as well as you do at home because you’re in a different place, but that’s okay. The test still works even if you don’t sleep the whole night.
-
Ending the Test: When you wake up in the morning, the technician takes off all the sensors. You can then leave the sleep center and go about your day as usual.
What happens after a polysomnography?
After you do a polysomnography (a sleep test), here’s what might happen:
-
Sleep Apnea Diagnosis: If you’re diagnosed with sleep apnea, your doctor might suggest using a CPAP machine. This machine gives you a steady flow of air through your nose or mouth while you sleep. They might do another test (polysomnography) to figure out the best settings for your CPAP machine.
-
Other Sleep Disorders: If you’re diagnosed with a different sleep problem, your doctor will talk to you about how to treat it. They’ll go over your options for feeling better while you sleep.
What are the risks associated with Polysomnography?
Polysomnography usually doesn’t have any risks. But sometimes, a person might have a reaction to the sticky stuff that holds the sensors on their body. If they’re worried about this, they can talk to the person running the test before it starts.
How much does Polysomnography cost?
The cost of polysomnography can vary. If you have Medicare, you might pay 20% of the Medicare-approved amount after you’ve paid your deductible. The final cost also depends on:
- Any other insurance you have.
- The type of facility where the sleep study happens.
- How much your doctor charges.
Who does a sleep study?
During a sleep study, different healthcare pros pitch in. You’ll likely meet medical technicians, technologists, assistants, and nurses, including registered and licensed practice nurses.
Once your sleep study wraps up, a doctor—like a pulmonologist or sleep medicine specialist—takes over. They sift through the test records for any red flags. Sometimes, they team up with other specialists, such as neurologists or your primary care doc, to gather more details about your health. They might also loop in your regular doctor to ensure everyone’s on the same page for your care.
At-home sleep apnea testing vs Sleep Study
An at-home sleep apnea test is similar to a sleep study, but they’re not exactly the same. Unlike a full sleep study, the at-home version usually doesn’t use all the fancy sensors. Some sensors, like the ones for brain waves, eye movement, or heart activity, might be skipped.
Instead, the at-home test focuses on simpler sensors. These check things like how you breathe through your nose or mouth and if your chest and belly muscles move when you breathe. It’s often done when the doctor strongly thinks you have sleep apnea or as a follow-up after treatment to see if it’s still there.
What do the sleep study results mean?
When you get your PSG results, it might take around 3 weeks. A technician will put together the data from your sleep study night to make graphs showing your sleep patterns. Then, a sleep center doctor will check out this info along with your medical and sleep history to figure out what’s going on.
If your PSG results are not normal, it could mean you have sleep-related problems like:
- Sleep apnea or other breathing issues
- Seizure disorders
- Movement problems like periodic limb movement disorder
- Conditions causing unusual daytime tiredness like narcolepsy
To find out if you have sleep apnea, the doctor will look at the PSG results to see:
- How often you stop breathing for 10 seconds or more (apnea episodes)
- How often your breathing is partially blocked for 10 seconds or more (hypopnea episodes)
Using this info, the doctor calculates something called the apnea-hypopnea index (AHI). If your AHI score is under 5, it’s normal. This, plus normal brain and muscle data, usually means no sleep apnea.
But if your AHI score is 5 or more, it’s not normal. Your doctor will then look at how severe your sleep apnea is:
- A score of 5 to 15 means mild sleep apnea
- A score of 15 to 30 means moderate sleep apnea
- A score higher than 30 means severe sleep apnea
For mild cases of sleep apnea, you can consider using some anti-snoring devices or anti-snoring mouthpieces.
FAQs
1. How long does a sleep study last?
Usually, just one night in a sleep lab is enough for most people. If it’s a daytime study, it’s about the equivalent of a night’s sleep. Experts say sleeping for at least two hours is needed for a valid study. However, sleeping more like usual gives better data.
2. Will someone watch me during the study?
There are cameras, but staff don’t watch you constantly. Cameras are mainly there to check if something unusual happens or to match recordings with sensor data.
3. Can I use the bathroom during the study?
Yes, you can. But rules may vary depending on the lab’s setup. The staff will let you know what’s allowed.
4. Do I have to do the study alone?
Yes, usually. Exceptions are made for children or special cases, but they might need a separate room to avoid affecting the results.
5. Does a sleep study hurt?
No, it’s painless. The sensors and equipment used won’t cause any discomfort. Removing sensors might cause slight discomfort, but staff can help minimize it.